Opioid-Induced Hyperalgesia: Recognizing and Managing This Paradoxical Pain Condition
Imagine taking opioids for pain relief, only to find your pain getting worse. That's the paradox of opioid-induced hyperalgesia, a condition where the very drugs meant to ease pain actually heighten sensitivity to it. First scientifically documented in 1971, Opioid-Induced Hyperalgesia (OIH) a paradoxical state where opioid exposure increases pain sensitivity affects 2-15% of chronic opioid users. Unlike opioid tolerance, where higher doses temporarily restore pain relief, OIH causes pain to intensify with each dose increase. Understanding this condition is critical for effective pain management.
What is Opioid-Induced Hyperalgesia?
Opioid-Induced Hyperalgesia a condition where opioids paradoxically increase pain sensitivity occurs when the body becomes overly sensitive to pain after opioid exposure. While opioids typically block pain signals, they can sometimes trigger a counterintuitive response. This phenomenon was first observed in animal studies by Eddy et al. in 1971, where repeated morphine injections caused hyperalgesia in rats. Today, clinical evidence confirms OIH affects humans too, especially those on long-term opioid therapy for chronic pain.
Pain specialists now recognize OIH as a distinct clinical entity separate from tolerance or disease progression. According to the Palliative Care Network of Wisconsin a resource for clinical guidance in palliative care's Fast Fact #142 (2024), OIH manifests when patients experience worsening pain despite escalating opioid doses. This is a key diagnostic clue - if pain gets worse with higher doses, OIH may be the culprit.
Symptoms and Signs of OIH
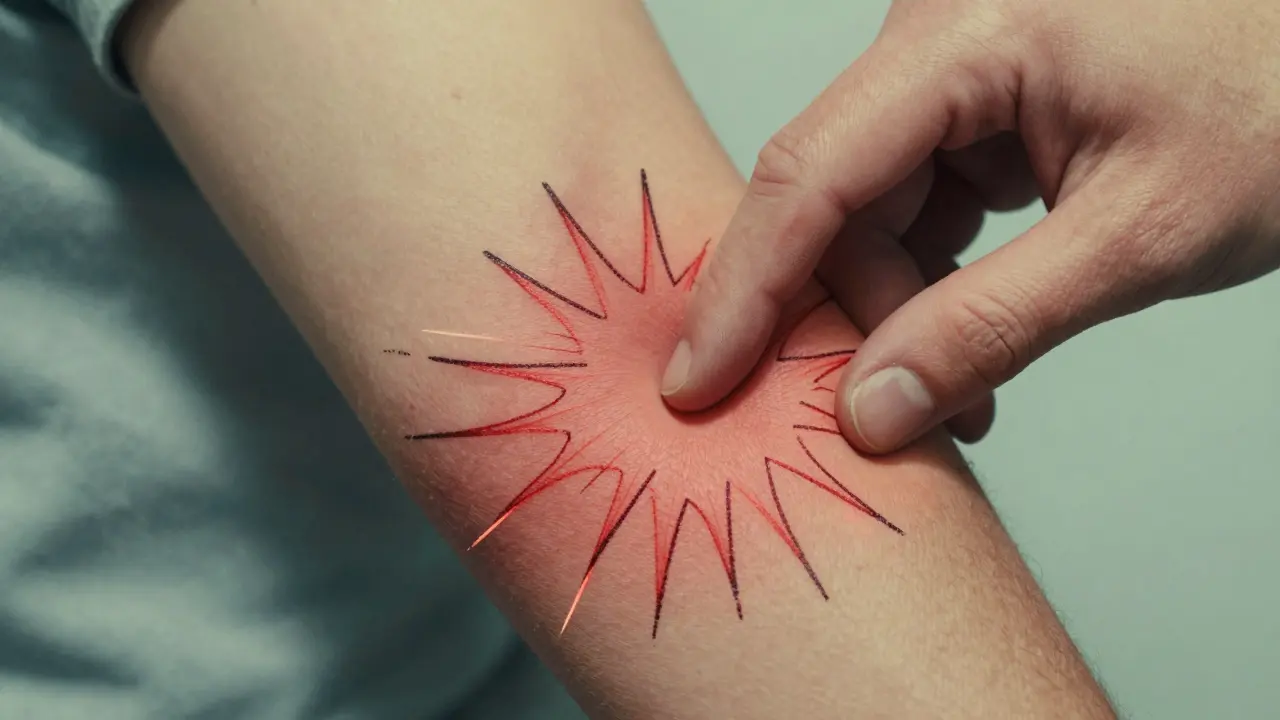
Patients with OIH often report pain that spreads beyond the original injury site. For example, someone with back pain might start feeling discomfort in their legs or feet without any new physical damage. This diffuse pain pattern is a red flag. Another hallmark symptom is allodynia pain from stimuli that shouldn't cause pain, like light touch. Simple things like clothing rubbing against skin or a breeze can become painful. These symptoms don't improve with more opioids - they often get worse.
Unlike typical pain conditions, OIH pain is unpredictable. Patients might describe their pain as "burning" or "shooting" in areas unrelated to their original problem. Clinical studies show OIH can occur at any opioid dose, but it's most common with high-dose morphine (over 300mg/day) or hydromorphone, especially in patients with kidney issues where metabolites build up.
How OIH Differs from Tolerance
Many clinicians confuse OIH with opioid tolerance, but they're fundamentally different. Pain tolerance reduced response to opioids requiring higher doses for effect means patients need more medication to achieve the same pain relief. However, their pain doesn't worsen overall - it's just harder to control. In OIH, the opposite happens: higher doses make pain feel more intense.
| Feature | OIH | Tolerance |
|---|---|---|
| Pain response to higher doses | Worsens | Improves temporarily |
| Pain distribution | Diffuse, spreads beyond original area | Localized to original pain site |
| Allodynia | Common (pain from light touch) | Rare |
| Primary mechanism | NMDA receptors glutamate receptors involved in pain sensitization activation | Opioid receptor desensitization |
| Treatment approach | Reduce dose, switch opioids, add ketamine | Gradual dose increase |
Causes and Mechanisms
The exact causes of OIH remain complex, but research points to several neurobiological pathways. The most significant mechanism involves NMDA receptors glutamate receptors that become overactivated by opioids in the spinal cord. When opioids bind to these receptors, they trigger a cascade that amplifies pain signals instead of blocking them.
Other factors include toxic opioid metabolites. For example, morphine breaks down into morphine-3-glucuronide, which can activate pain pathways. Similarly, hydromorphone produces hydromorphone-3-glucuronide. Patients with kidney problems are especially vulnerable because these metabolites accumulate. Genetic factors also play a role - variations in the COMT gene affect how the body processes opioids, making some individuals more prone to OIH.
Diagnosing OIH
Diagnosing OIH requires careful assessment to rule out other causes of worsening pain. Doctors look for specific red flags: pain that spreads beyond the original site, allodynia, and worsening symptoms despite higher opioid doses. The Opioid-Induced Hyperalgesia Questionnaire (OIHQ) validated clinical tool for OIH diagnosis has been shown to identify OIH with 85% accuracy. This tool asks about pain patterns and responses to dose changes.
Quantitative sensory testing (QST) can also help. This involves measuring how patients respond to controlled pain stimuli before and after opioid administration. In OIH patients, pain thresholds typically decrease - meaning they feel pain more easily. However, this test isn't widely available, so clinical judgment remains key.

Management Strategies for OIH
The cornerstone of OIH treatment is reducing opioid exposure. Clinicians typically start by lowering the current dose by 10-25% every 2-3 days. For example, if a patient is taking 100mg of morphine daily, reducing to 75-90mg can help reverse symptoms. In some cases, completely stopping opioids may be necessary.
Switching opioids is another effective strategy. Methadone an opioid with NMDA-blocking properties is often used because it blocks NMDA receptors. Buprenorphine a partial opioid agonist with NMDA antagonism is another option. Both have shown success in managing OIH while maintaining pain control.
Adding non-opioid medications is critical. Ketamine NMDA receptor antagonist used at sub-anesthetic doses at 0.1-0.5 mg/kg/hour intravenously has demonstrated rapid reversal of OIH symptoms. Gabapentin medication targeting nerve-related pain (300-1800mg daily) and Clonidine alpha-2 agonist for pain modulation (0.1-0.3mg twice daily) also target the underlying mechanisms of OIH. These medications work together to calm the nervous system.
Practical Steps for Clinicians
Implementing OIH management requires a structured approach. First, assess the patient's pain pattern and opioid history. If pain worsens with dose increases and shows diffuse allodynia, suspect OIH. Reduce the opioid dose immediately - don't escalate further. Monitor symptoms over 2-4 weeks for improvement. If pain persists, consider switching opioids or adding ketamine.
Common challenges include patient resistance to dose reduction. About 40-60% of patients fear their pain will return without higher doses. Clear communication is essential - explain that reducing opioids may actually relieve their pain. Also, distinguish OIH from withdrawal symptoms, which typically involve nausea, sweating, and anxiety. OIH symptoms are purely pain-related and worsen with more opioids.
Most patients see improvement within 2-4 weeks of dose adjustment. Complete resolution usually takes 4-8 weeks. The National Comprehensive Cancer Network (NCCN) Adult Cancer Pain Guidelines (v3.2024) provide detailed protocols for OIH management, including step-by-step dose reduction schedules and alternative medication options.
Frequently Asked Questions
Can OIH be mistaken for opioid tolerance?
Yes, OIH and tolerance share similar symptoms like needing higher doses for pain relief. However, in OIH, pain worsens with dose increases, whereas tolerance may temporarily improve with higher doses. Doctors often use the Opioid-Induced Hyperalgesia Questionnaire (OIHQ) to differentiate between the two.
How long does it take to recover from OIH?
Recovery varies, but most patients see improvement within 2-4 weeks of dose reduction or switching opioids. Complete resolution usually takes 4-8 weeks. Factors like the type of opioid used and the patient's overall health influence this timeline.
Is OIH reversible?
Yes, OIH is reversible with appropriate treatment. Reducing opioid doses, switching to alternative opioids like methadone, or adding ketamine can resolve symptoms. Clinical studies show over 70% of patients experience significant pain relief after implementing these strategies.
Can OIH occur with low-dose opioids?
While OIH is more common with high doses (over 300mg morphine/day), it can occur at lower doses too. Patients with kidney problems or specific genetic factors are at higher risk even with standard doses. Always monitor for symptoms regardless of opioid dosage.
What happens if OIH is left untreated?
Untreated OIH can lead to a dangerous cycle of increasing opioid doses, worsening pain, and higher risk of side effects like respiratory depression or addiction. It also complicates pain management for other conditions. Early recognition and treatment prevent these complications and improve quality of life.




9 Comments
Matthew Morales
February 6 2026This is super important! 😅 I had no idea opioids could make pain wrose. My buddy's been struggling with this. Gotta share this with my doc
Kate Gile
February 7 2026I've seen this firsthand in my practice. When patients report worsening pain with higher doses, we immediately consider OIH. Reducing the dose often helps. It's a game-changer for chronic pain management. I once had a patient who was on high-dose morphine for years. Every time we increased the dose, their pain got worse. We thought it was tolerance, but after reviewing the literature, we suspected OIH. We reduced the dose by 25% and started gabapentin. Within two weeks, their pain improved significantly. It's crucial for doctors to recognize OIH instead of just upping the dose. This condition is often misdiagnosed as tolerance, but the mechanisms are different. OIH involves NMDA receptor activation, while tolerance is about receptor desensitization. Proper diagnosis can save patients from unnecessary dose escalation and potential side effects. I always check for diffuse pain and allodynia. These are red flags for OIH. It's amazing how much we've learned about opioid-related issues in recent years. We need more education on this topic for healthcare providers. This article does a great job explaining it.
Gregory Rodriguez
February 8 2026Yeah, it's like the universe's cruel joke. Painkillers causing more pain. Classic. But hey, at least we're learning about it now.
Pamela Power
February 8 2026Actually, most cases of 'OIH' are just tolerance misdiagnosed. The real issue is poor clinical judgment. Most patients don't need opioids at all. This article is oversimplified.
anjar maike
February 10 2026Interesting 😊 OIH is common Any studies from India
Carl Crista
February 11 2026Big Pharma knows about OIH but hides it to keep selling opioids They don't want you to know the truth It's all about profits
Jenna Elliott
February 12 2026Doctors are useless Opioids should be banned All of them This is why I don't trust the medical system
Phoebe Norman
February 12 2026NMDA receptor involvement is key but often overlooked Morphine metabolites exacerbate this Clinicians must monitor closely
Albert Lua
February 14 2026In my country we use alternative meds like turmeric for pain But opioids are still common This OIH thing is a real issue globally