Hemochromatosis: Iron Overload and Phlebotomy Treatment Explained
Hemochromatosis isn't just a rare genetic quirk - it's a silent killer that quietly damages your liver, heart, and pancreas for years before you even notice something's wrong. Imagine your body absorbing iron like a sponge, even when you don't need it. That's what happens in hemochromatosis. Your body can't turn off iron absorption, so over time, excess iron piles up in your organs. Left untreated, this leads to cirrhosis, diabetes, heart failure, and even liver cancer. But here's the good news: if caught early, it's one of the easiest serious conditions to treat. All it takes is a simple procedure most people think is just for donating blood.
What Exactly Is Hemochromatosis?
Hemochromatosis is a genetic disorder where your body absorbs too much iron from food. It's not caused by eating too much red meat or taking iron supplements - it's built into your DNA. The most common form, called Type 1, comes from mutations in the HFE gene. Specifically, if you inherit two copies of the C282Y mutation (one from each parent), you have a very high chance of developing iron overload. This version affects about 1 in 200 people of Northern European descent. In places like Ireland, Scotland, and Wales, it's even more common - 1 in 83 people carry the double mutation.
Why does this happen? Normally, your liver makes a hormone called hepcidin that tells your gut when to stop absorbing iron. In hemochromatosis, that signal breaks down. Your intestines keep pulling iron in, your liver keeps storing it, and your body has no way to get rid of the excess. Iron isn't like water - you can't pee it out or sweat it out. The only natural way to lose it is through blood loss. That’s why women who menstruate often don’t show symptoms until after menopause. Men, on the other hand, start building up iron in their 30s and often don’t realize anything’s wrong until their 40s or 50s.
How Do You Know You Have It?
The scary part? Early symptoms are vague and easily mistaken for other things. You feel tired all the time? Maybe it’s stress. Your knees and knuckles ache? Must be aging. You’ve lost interest in sex? Probably just life getting busy. But these are the top three signs of early hemochromatosis - fatigue (74% of patients), joint pain (65%), and low libido (54%).
As it progresses, you might notice your skin turning a bronze or grayish color - not from sun exposure, but from iron deposits. You could develop abdominal pain, diabetes (25% of cases), or even heart rhythm problems. By the time these show up, your liver may already be scarred. That’s why blood tests are critical.
The two key tests are serum ferritin and transferrin saturation. Ferritin is your body’s iron storage marker. In men, levels over 300 ng/mL are a red flag. In women, over 200 ng/mL. Transferrin saturation measures how much iron is floating in your blood. A reading above 45% is abnormal. If both are high, and you have a family history or symptoms, genetic testing for HFE mutations confirms it. A ferritin level above 1,000 ng/mL means you’re at high risk for cirrhosis - and that’s when survival rates drop sharply.
Why Phlebotomy Is the Gold Standard Treatment
Here’s the beautiful irony: the best treatment for iron overload is removing blood. It’s called therapeutic phlebotomy. Think of it like donating blood - except it’s medical, not voluntary. Each time you give 450-500 mL of blood, you lose about 200-250 mg of iron. Your body responds by pulling iron out of your organs to make new red blood cells. Slowly, over time, your iron stores drop.
The treatment has two phases. First, the induction phase: you go to the clinic every week and give a unit of blood. This continues until your ferritin hits 50 ng/mL. For someone with ferritin at 2,500 ng/mL (not uncommon), that can take 12 to 18 months - sometimes over 60 sessions. One Reddit user, u/HemoWarrior, shared that after 8 years of misdiagnosis, he needed 62 phlebotomies over 15 months to get his levels down.
Then comes the maintenance phase. Once you’re at target levels, you don’t stop. You keep giving blood every 2 to 4 months to stay in the safe range of 50-100 ng/mL. Most people need 4 to 6 sessions a year. This isn’t optional. If you stop, your iron creeps back up, and damage resumes.
It’s cheap, too. Each session costs $0-$50, often covered by insurance. Compare that to iron-chelating drugs like deferasirox, which cost $25,000-$35,000 a year and come with nasty side effects. Phlebotomy is the only treatment that’s effective, safe, and free of long-term toxicity.

What Happens If You Don’t Treat It?
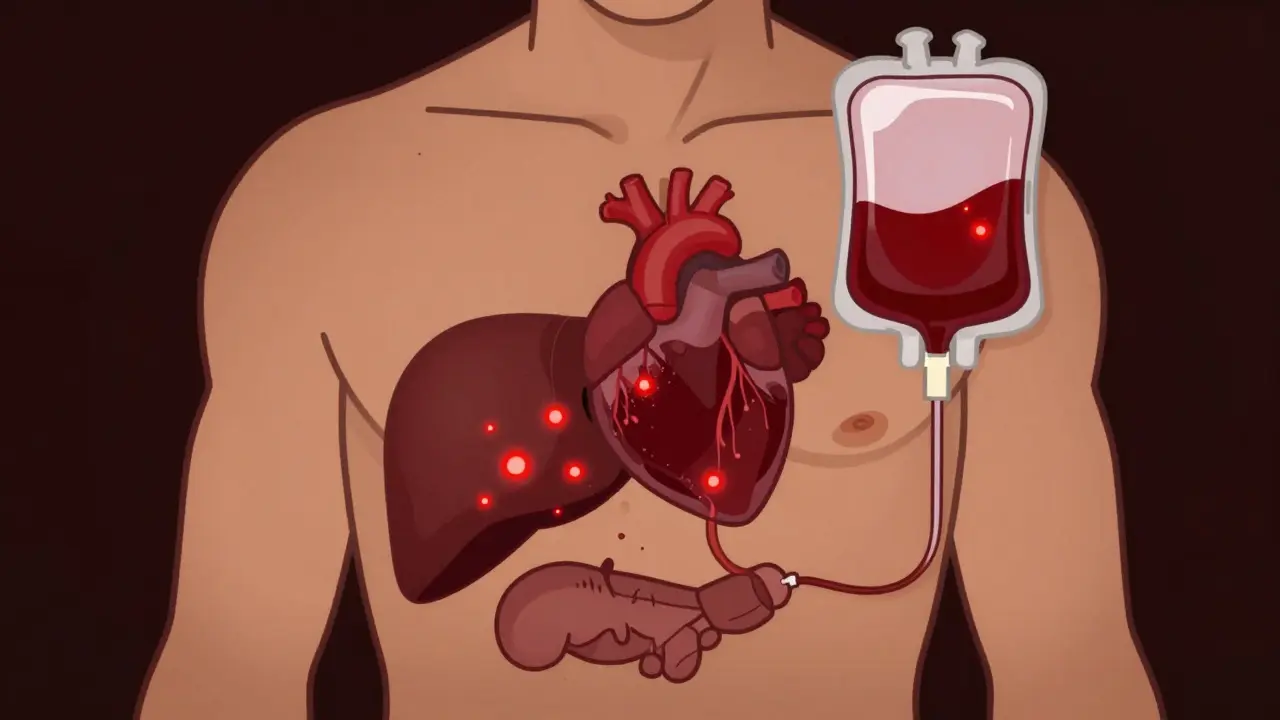
Untreated hemochromatosis doesn’t just make you tired - it destroys organs. The liver is ground zero. Iron builds up in liver cells, triggering inflammation, fibrosis, and eventually cirrhosis. Once cirrhosis sets in, your risk of liver cancer skyrockets. Studies show that if your ferritin is over 1,000 ng/mL at diagnosis, you have a 50-75% chance of already having cirrhosis. Your 10-year survival rate drops from 95% to 60%.
Iron also wrecks the pancreas. It damages insulin-producing beta cells, leading to diabetes. In fact, about 1 in 4 people with hemochromatosis develop diabetes before they’re even diagnosed. The heart isn’t safe either - iron can cause arrhythmias and heart failure. And yes, it affects your hormones too. Low testosterone in men and early menopause in women are common.
Dr. Paul Adams, a leading researcher, says: “Early diagnosis and treatment before ferritin exceeds 1,000 ng/mL can prevent 99% of cirrhosis and liver cancer.” That’s not a guess - it’s data from thousands of patients tracked over decades.
Why Diagnosis Takes So Long
Most patients see 3 to 5 doctors over 5 to 7 years before getting the right diagnosis. Why? Because doctors don’t test for it. A 2023 study found only 12% of primary care physicians routinely check transferrin saturation when someone complains of fatigue or joint pain. They assume it’s depression, arthritis, or aging.
And even when they do test, they misread the results. Some think a normal CBC (complete blood count) rules out iron overload. It doesn’t. You can have high ferritin and normal hemoglobin. Others think you need to be anemic to need phlebotomy. Again, wrong. The goal is to get your iron down, not to treat anemia.
Family history is the biggest clue. If your parent or sibling has it, your risk jumps dramatically. The Hemochromatosis Foundation says 70% of diagnosed cases come from testing relatives after one person is found. That’s why cascade screening - testing first-degree relatives - is so powerful.
What About New Treatments?
There’s exciting research happening. Scientists are developing hepcidin mimetics - drugs that trick your body into thinking it has enough iron. One drug, PTG-300, showed a 53% drop in transferrin saturation in just 12 weeks during a 2023 clinical trial. That could mean fewer blood draws in the future.
But here’s the catch: these drugs aren’t approved yet. And even if they were, they’d cost thousands a month. Phlebotomy still works better, cheaper, and with zero side effects. MRI scans can now measure liver iron without a biopsy, making monitoring safer and more accurate. But none of this changes the core truth: if you have hemochromatosis, phlebotomy is still your best, most proven option.
Real-Life Challenges
It’s not all smooth sailing. Many patients struggle with access. Blood donation centers often refuse therapeutic phlebotomy because they’re set up for voluntary donors. You have to find a hospital or specialized clinic. Some patients over 50 have hard-to-access veins. Others get tired of the routine. One survey found 42% of patients experience “treatment fatigue” after a few years - they stop going because they feel fine. But feeling fine doesn’t mean your iron is under control.
And insurance? It varies. Some plans cover it fully. Others require pre-authorization. Always check with your provider. If you’re having trouble, the American Hemochromatosis Society can help connect you with clinics that accept therapeutic donations.
What You Can Do Today
If you’re tired all the time, have unexplained joint pain, or have a family history of liver disease, diabetes, or heart problems - ask your doctor for two simple tests: serum ferritin and transferrin saturation. Don’t wait for symptoms to get worse. If your ferritin is over 300 (or 200 if you’re female), get genetic testing. If you’re diagnosed, start phlebotomy immediately. Don’t delay. The earlier you begin, the more of your organs you save.
And if you’ve been diagnosed? Stick with it. Keep your maintenance sessions. Your liver will thank you. Your heart will thank you. Your future self will thank you.
Can you get hemochromatosis from eating too much iron?
No. Hemochromatosis is genetic. You can’t get it from diet, supplements, or cooking with iron pans. Your body absorbs iron uncontrollably because of a faulty gene - not because you’re eating too much. In fact, people with hemochromatosis are often told to avoid iron-rich foods, but that alone won’t stop the overload. Treatment requires removing blood, not changing your diet.
Is phlebotomy dangerous or painful?
It’s very safe. It’s the same process as donating blood. You might feel a little lightheaded afterward, especially if you’re low on fluids. Some people get a small bruise or soreness at the needle site. But serious complications are rare. Most patients say it’s no worse than a routine blood test. The real risk is not doing it - not the procedure itself.
Can women get hemochromatosis?
Yes. While men are diagnosed more often - and earlier - because they don’t lose iron through menstruation, women absolutely get it. Symptoms usually appear after menopause, when iron storage starts climbing. Women with the double HFE mutation can develop severe iron overload, liver damage, and diabetes just like men. Don’t assume it’s a “man’s disease.”
Do I need to avoid alcohol if I have hemochromatosis?
Yes. Alcohol increases iron absorption and damages the liver. If you already have iron overload, alcohol speeds up scarring and raises your risk of cirrhosis and liver cancer. Even moderate drinking - one drink a day - can be harmful. Doctors recommend complete abstinence for people with hemochromatosis, especially if ferritin is high or liver damage is present.
Can I still donate blood after being diagnosed?
Yes - and you should. Once you’re in maintenance, you can often donate blood at your local blood center. Many centers now accept therapeutic donations from hemochromatosis patients. It’s a win-win: you stay healthy, and your blood helps someone else. Check with your doctor and local blood bank - some require a letter from your physician, but most are happy to help.
What if I have the gene but no symptoms?
You still need treatment. Many people with the double mutation feel fine for years - until they suddenly don’t. Iron builds up slowly. By the time symptoms appear, organs may already be damaged. If you have the HFE mutation and your ferritin is above 300 ng/mL (or 200 for women), start phlebotomy now. Waiting for symptoms is like waiting for a fire alarm to go off before you put out the smoke.



14 Comments
Agbogla Bischof
March 25 2026Interesting breakdown-especially the part about hepcidin signaling. I’ve seen this in my endocrinology work: patients with elevated ferritin are often mislabeled as ‘metabolically unhealthy’ when it’s actually genetic iron overload. The key is testing transferrin saturation early, not just ferritin. Many clinicians don’t realize ferritin can be normal in early stages if there’s inflammation masking it.
Pat Fur
March 27 2026I love how you framed this. It’s not just a medical condition-it’s a silent thief. And phlebotomy? It’s poetic. Taking blood to give life back.
peter vencken
March 28 2026my doc told me to cut back on steak and iron cereal. i was like… bro i’ve been getting blood drawn since 2018. turns out i had two copies of c282y. now i feel like a new person. no more brain fog. also, i donate at the red cross now. win-win.
Chris Crosson
March 30 2026I’ve been doing maintenance phlebotomy for 7 years. It’s not glamorous, but it’s the only thing keeping me alive. My ferritin was 3,200 when diagnosed. Now it’s stable at 80. I’m 41. My liver’s fine. My heart’s fine. Don’t wait until you’re in crisis.
Linda Foster
March 30 2026While the clinical data presented is compelling, I must emphasize the ethical imperative of cascade screening. Genetic conditions such as this demand proactive familial evaluation, not merely reactive clinical intervention. The cost-benefit analysis strongly favors early detection.
Rama Rish
March 30 2026my aunt had this and no one knew. she got liver transplant at 52. now we all get tested. if you have family history? just do it. easy blood test. save yourself.
Darlene Gomez
March 31 2026There’s something deeply human about this-how a simple act of blood removal becomes a lifeline. We fear what we can’t see, but here, the cure is as old as medicine itself: restore balance. Not by drugs, not by restriction, but by letting go. Quietly. Regularly. Gently.
Stephen Alabi
April 1 2026While your article is superficially informative, it lacks critical nuance. The assertion that phlebotomy is 'the only effective treatment' ignores emerging hepcidin agonists currently in Phase III trials. Furthermore, your dismissal of dietary modification is scientifically unsound-vitamin C enhances non-heme iron absorption, and excessive alcohol consumption synergistically accelerates hepatic damage. The narrative of 'just bleed and you're fine' is dangerously reductive.
Kevin Siewe
April 3 2026Thank you for writing this. I was diagnosed at 38 after years of being told I was 'just stressed.' I thought I was fine because I didn't feel sick. Turns out, my liver was already 30% fibrotic. I started phlebotomy. Now I go every 3 months. I sleep better. I have energy. I'm not 'cured'-but I'm not dying either. This isn't about fixing a disease. It's about preserving a life.
Natasha Rodríguez Lara
April 3 2026My mom’s from Ireland. We all got tested after my uncle got liver cancer. I had the mutation. I started phlebotomy at 29. I’m 36 now. No symptoms. No damage. I feel like I got a second chance because someone finally asked the right question. If you’re tired and your family’s from Northern Europe? Don’t wait. Ask.
Chris Farley
April 3 2026This is what happens when you let genetics dictate health. Why not just ban iron-rich foods? Or make everyone take chelators? Why are we normalizing a system where you have to bleed yourself to stay alive? It’s a failure of modern medicine. We should be fixing the gene-not draining blood like it’s 1890.
Anil Arekar
April 4 2026As a physician in India, I rarely see hemochromatosis, but the principles remain universal. Iron overload is not exclusive to Northern European populations-secondary causes exist. However, the genetic form, when present, demands the same vigilance. Early testing, consistent monitoring, and adherence to maintenance phlebotomy are non-negotiable. This condition does not discriminate by geography-it only discriminates by awareness.
Katie Putbrese
April 5 2026Why are we letting people with this condition donate blood? It’s a genetic defect. It’s not 'healthy' blood. And why aren’t we screening everyone at birth? This is a public health failure. If your DNA says you’re a walking iron bomb, you shouldn’t be allowed to reproduce or donate plasma. We’re too soft on genetic risk.
Elaine Parra
April 6 2026My husband had this. We found out after his heart started failing. He needed 87 phlebotomies. He’s alive because we acted fast. If you have fatigue, joint pain, or low libido-don’t shrug it off. Get tested. Your life isn’t a waiting game. It’s a countdown.