How to Store Light-Sensitive Medications and Eye Drops Properly
Storing light-sensitive medications and eye drops wrong can make them useless-or even dangerous. You might not realize it, but sunlight, even through a window, can break down your medicine over time. That $80 bottle of eye drops? It could lose half its strength in just two weeks if left on the bathroom counter. And it’s not just eye drops. Antibiotics, birth control pills, chemotherapy drugs, and even vitamin D drops can degrade when exposed to light. The result? Your treatment doesn’t work like it should. That’s not speculation-it’s science.
What Makes Medications Light-Sensitive?
Some medicines contain chemicals that react when hit by certain wavelengths of light, especially UV and blue light. This reaction changes their structure. For example, tetracycline antibiotics can turn toxic. Nitroglycerin, used for chest pain, loses its ability to open blood vessels. Eye drops like latanoprost (used for glaucoma) can become less effective, putting your vision at risk. The pharmaceutical industry has known this for over a century. Back in the 1920s, pharmacists noticed that certain drugs turned brown or cloudy when left in sunlight. That’s why amber bottles became standard.
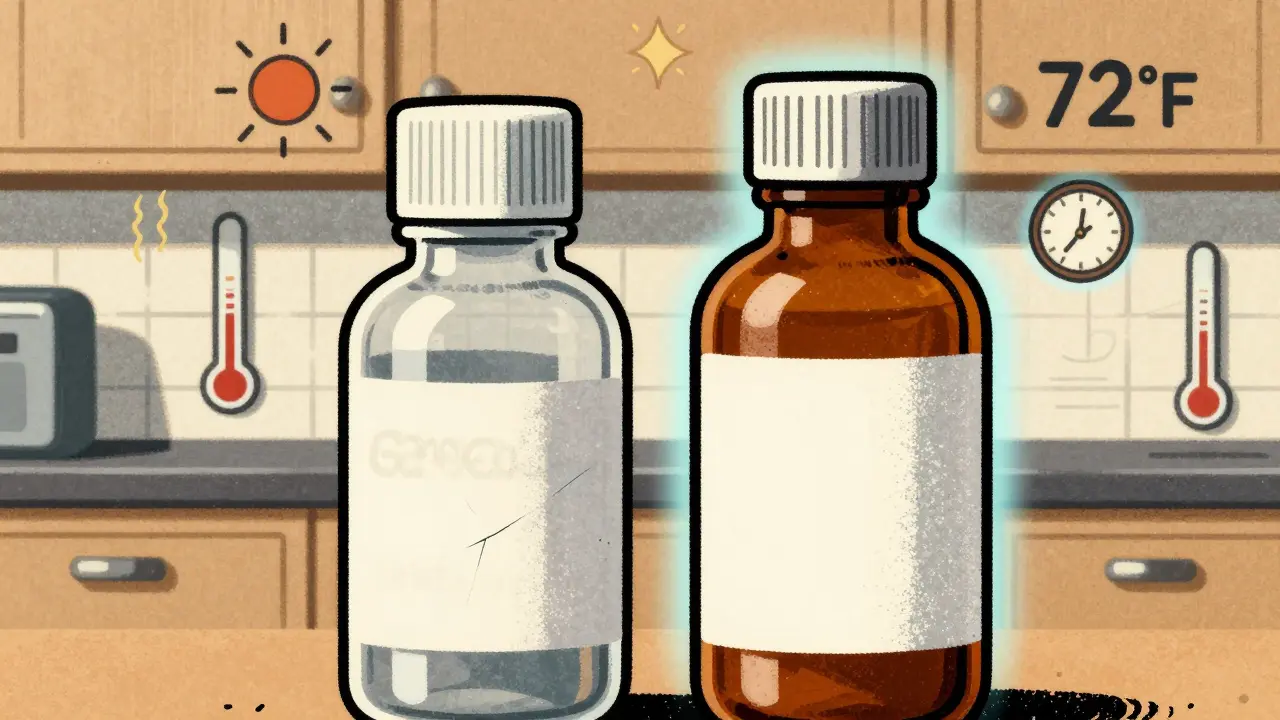
Today, the United States Pharmacopeia (USP) requires that light-sensitive drugs be packaged in containers that block light below 470 nanometers. That’s the range where most degradation happens. Amber glass blocks 98% of this harmful light. High-quality opaque plastic blocks about 85%. The difference might sound small, but for something as precise as eye drops, it matters. A 2021 study from Alcon showed that eye drops stored in clear containers lost 35% of their potency in just 14 days. In amber bottles? Almost none.
Where Should You Store Them?
Your medicine cabinet is probably the worst place. Bathrooms are hot, humid, and full of light from overhead fixtures. A 2022 survey by the National Community Pharmacists Association found that 68% of people store meds there-and 42% noticed discoloration or texture changes. That’s not normal. It’s degradation.
Instead, pick a cool, dry spot away from windows. A kitchen cabinet, far from the stove or sink, works well. The ideal temperature range is 59-77°F (15-25°C). Most medications are fine within 58-86°F, but why risk it? If your home gets hot in summer, especially if you don’t have AC, that 86°F line becomes a real problem. The InfantRisk Center says exceeding 86°F can permanently alter how your meds work.
For eye drops, once opened, they should stay between 40-77°F. That means you can keep them at room temperature, but don’t leave them on the windowsill. Some eye drops, like certain antibiotics or biologics, need refrigeration. Check the label. If it says “refrigerate,” keep them between 36-46°F. Never freeze them.
What About the Original Container?
Never transfer eye drops or light-sensitive meds to another bottle-unless it’s a proper amber one. That old contact lens case? A plastic pill organizer? A clear Tupperware? They offer zero protection. A 2023 study from the American Academy of Ophthalmology found that 18% of eye treatment failures were caused by patients moving drops into non-protective containers.
Keep meds in their original packaging. Those amber bottles aren’t just for looks-they’re engineered to last. Some even have UV-blocking coatings inside the plastic. Brands like Bausch + Lomb and Alcon design multi-dose eye drop containers with dual protection: amber glass plus an opaque outer layer. These last 25% longer than standard amber bottles.
If your bottle is clear and the label says “protect from light,” call your pharmacist. They can often swap it for a proper one at no cost. Some pharmacies even offer free opaque sleeves you can slip over clear bottles.
Special Cases: Insulin, Biologics, and Chemotherapy
Not all light-sensitive meds are the same. Insulin, for example, needs both cold and dark. Unopened insulin vials go in the fridge. Once opened, they can stay at room temperature for up to 28 days-but still away from direct light. A 2022 report from the Pharmaceutical Research and Manufacturers of America (PhRMA) found that 78% of light-sensitive medications need protection during storage, and 32% need it during use.
Biologics-like those for rheumatoid arthritis or multiple sclerosis-are even more fragile. They’re made from living cells and can break down quickly. Many require refrigeration AND complete darkness. That’s why some come in special insulated boxes with built-in UV filters. These cost more, but they’re worth it. One study showed they maintain stability for 28 days versus 14 days in regular coolers.
Chemotherapy drugs are another high-risk category. The US Pharmacist lists potassium iodide, tinctures, and certain chemo agents as “extremely light-sensitive.” Even a few minutes of light exposure during preparation can reduce effectiveness. Always follow your oncology nurse’s instructions to the letter.
Traveling with Light-Sensitive Medications
Traveling? Pack smart. A regular suitcase won’t cut it. The FDA recommends insulated medication bags with UV-blocking lining. These keep meds at stable temps for 8-12 hours-even in hot cars or sunny airports.
Some patients use small, portable coolers with ice packs. But don’t let the meds freeze. Wrap them in a towel first. Another trick: keep them in your carry-on, not checked luggage. Baggage holds can get hotter than 120°F.
For long trips, consider a smart storage device. MedMinder is testing a prototype container with a built-in UV sensor. It sends an alert to your phone if the meds get too much light. It’s not widely available yet, but it’s coming.
How to Tell If Your Medicine Has Gone Bad
Signs of degradation are easy to spot if you know what to look for:
- Eye drops: Cloudy, discolored (yellow or brown), or have floating particles
- Topical creams: Changed color (white turning yellow), oily separation, or strange smell
- Pills: Cracked, chipped, or stained
- Insulin: Cloudy when it should be clear (or vice versa)
Aspirin that smells like vinegar? That’s acetic acid forming-proof it’s broken down. Tetracycline that’s darkened? Don’t take it. It can damage your kidneys.
If you notice any of this, stop using it. Call your pharmacist. Don’t guess. They can tell you if it’s still safe or if you need a replacement.
What Storage Solutions Work Best?
Here’s a quick breakdown of your options:
| Option | Light Protection | Temp Stability | Cost | Pros | Cons |
|---|---|---|---|---|---|
| Amber glass bottle | 98% | Good | $0.08-$0.20/unit | Continuous protection, no user action needed | Hard to see how much is left |
| Opaque plastic bottle | 85% | Good | $0.15-$0.35/unit | Easier to read contents | Less durable, may degrade over time |
| Aluminum foil pouch | 100% | Poor | $0.20-$0.50/unit | Complete protection | Must remove meds before use-32% non-compliance rate |
| UV-blocking storage box | 95% | Good | $19.99-$59.99 | Stores multiple items, portable | Requires manual placement |
| Insulated travel bag | 90% | Excellent | $25-$45 | Perfect for trips, maintains temp | Only useful during travel |
For most people, the original amber bottle is still the best choice. It’s cheap, reliable, and designed for the job. If you can’t see how much is left, use a small piece of tape to mark the level. Or buy a pill organizer with a built-in light meter-some now come with them.
What Happens If You Don’t Store Them Right?
It’s not just about wasted money. A 2022 FDA MedWatch report recorded 1,842 adverse events linked to improper storage, with 327 specifically tied to light exposure. That’s not a small number. People got sicker. Infections didn’t clear. Glaucoma pressure spiked. Birth control failed.
One Reddit user, ‘MedTechRN,’ lost $120 worth of tretinoin cream because it turned yellow after sitting in a steamy bathroom. Another, ‘Eyesafe2022,’ said their glaucoma drops lasted the full 6 weeks-only because they kept them in the original amber bottle. That’s the difference between a treatment that works and one that doesn’t.
And it’s not just you. The American Society of Health-System Pharmacists (ASHP) says 37% of all medication efficacy complaints come from improper storage. Light exposure is the #1 culprit.
Final Tips: Simple Habits That Make a Big Difference
- Check every bottle for “protect from light” or a sun icon. If it’s there, treat it like a fragile item.
- Store meds in a drawer or cabinet, never on the counter or windowsill.
- Use a hygrometer if you’re unsure about humidity. High moisture speeds up degradation.
- Keep meds out of reach of kids and pets-child-resistant caps are great, but not foolproof.
- Don’t leave eye drops in your car, even in winter. Cold + light = double risk.
- When in doubt, throw it out. Medications aren’t worth the risk.
Proper storage takes less than a minute a day. But it can mean the difference between healing and worsening. Your medicine works better when you protect it-not just from germs, but from light, heat, and humidity too.
Can I store eye drops in the fridge?
Yes, if the label says to refrigerate. Most eye drops can be kept at room temperature after opening, but some-like certain antibiotics or biologics-need refrigeration. Always check the instructions. Never freeze eye drops. If refrigerated, let them sit for a few minutes before use to avoid discomfort from cold liquid.
How long do eye drops last after opening?
Most multi-dose eye drops last 4 to 6 weeks after opening, even if the bottle says “use by” a longer date. Light and bacteria can spoil them faster. Always write the opening date on the bottle. If it looks cloudy, smells odd, or has particles, toss it-even if it’s within the date.
Are clear plastic bottles okay for light-sensitive meds?
No. Clear plastic offers almost no protection. Even if it’s labeled “UV-resistant,” it’s not enough. Only use containers that are amber, opaque, or specifically labeled as light-protective. The USP requires light transmission below 10% for wavelengths 300-450 nm. Clear plastic allows up to 70% through.
What if I accidentally left my medicine in the sun?
If it was only a few hours, and the container was intact, it’s probably fine. But if it was days, or the medicine changed color or texture, don’t use it. For critical meds like insulin or chemotherapy, contact your pharmacist immediately. Better safe than sorry.
Can I use a regular pill organizer for light-sensitive meds?
Only if the pills are already in their original light-protected packaging. Never transfer eye drops, creams, or liquids into a clear pill organizer. The plastic won’t block light, and humidity can ruin them. For pills, choose an opaque organizer with a tight seal. But for anything liquid or topical, stick to the original container.





11 Comments
Ethan Zeeb
March 3 2026My ophthalmologist switched me to amber bottles after I lost vision in one eye from degraded glaucoma drops. I thought I was being careful-kept them in the cabinet-but the cabinet had a tiny window crack letting in blue light. Turned out, even indirect exposure was enough. Now I wrap mine in foil and store them in a black sock inside a drawer. Sounds weird, but it works. Don’t gamble with your sight.
Justin Rodriguez
March 3 2026As a pharmacist for 18 years, I’ve seen too many patients ruin their meds by storing them in bathrooms. The humidity alone kills stability, but light? That’s the silent killer. I hand out free opaque sleeves to anyone who brings in clear bottles. It’s not complicated-just don’t treat medicine like a decorative item. If it’s light-sensitive, treat it like a film negative. No exceptions.
Alex Brad
March 5 2026Amber bottle. Drawer. Done.
Renee Jackson
March 5 2026I cannot express how vital this information is. I recently helped my mother, who has diabetes and glaucoma, reorganize her medication storage after reading this. She had been keeping her insulin and eye drops side-by-side on the bathroom counter-she thought it was convenient. After implementing these guidelines, her HbA1c dropped by 0.8% and her eye pressure stabilized. This isn’t just advice-it’s life-saving protocol. Thank you for sharing this with such clarity and precision.
RacRac Rachel
March 6 2026OMG YES 😭 I used to keep my latanoprost on the windowsill because I forgot it was there-until one day it turned yellow and I had to rush to the ER because my eye pressure spiked. Now I have a tiny black box labeled "EYE MEDS - DO NOT TOUCH" under my sink. Also, I write the opening date on the bottle with a Sharpie. 💯 I even bought a UV light meter on Amazon to check my cabinet. It’s a little extra, but my vision? Priceless. 🙏
Jane Ryan Ryder
March 7 2026So let me get this straight-you’re telling me I need to baby my $80 eye drops like they’re a damn crystal? Grow up. If your medicine breaks because you left it in a drawer, you probably shouldn’t be taking it anyway. I keep mine in the glovebox. If it doesn’t work, I’ll just get more. Healthcare is a scam anyway.
Callum Duffy
March 8 2026While the American guidelines are thorough, I would note that in the UK, the NHS routinely provides light-protective storage bags for chronic ocular medications, particularly for patients on long-term glaucoma therapy. These are often distributed alongside prescription refills. Additionally, ambient temperature control is prioritized over light exposure in some NHS protocols, as humidity is considered a more consistent degrading factor in our climate. A nuanced approach is warranted.
Chris Beckman
March 9 2026bro i just throw all my stuff in a drawer and forget about it. i dont even look at the label. if it works, it works. if it dont, i go to cvs and get more. i mean, its not like my life depends on it. also why do people care so much about light? its just a bottle. you think the sun is gonna steal your medicine? lol. also i store my insulin in the garage. its fine.
Levi Viloria
March 10 2026There’s a cultural blind spot here. In many parts of the world-especially in rural communities-you don’t have cabinets, refrigerators, or even consistent electricity. The assumption that everyone can store meds in a climate-controlled drawer is a luxury mindset. I’ve seen grandparents in rural Tennessee keep their eye drops in Mason jars under the porch, shielded by old t-shirts. It’s not ideal, but it’s functional. Maybe the real issue isn’t storage-it’s access. If you can’t afford amber bottles or UV sleeves, then the system failed you long before the light got to the medicine.
Richard Elric5111
March 12 2026One must consider the ontological implications of pharmaceutical degradation. If a substance loses its efficacy due to photonic interference, does it retain its pharmaceutical identity? Or does it become something else-an inert residue, a phantom of its former function? The amber bottle, then, is not merely a container but a metaphysical boundary, a guardian against the entropy of therapeutic intention. To neglect its preservation is to commit a quiet epistemological violence upon the self. The medicine, in its degradation, whispers: "You were not worthy of healing." This is not science. This is ritual.
Dean Jones
March 13 2026Look, I get that this is important, but let’s be real-most people don’t live in sterile, climate-controlled labs. I live in a 1970s ranch house in Arizona with no AC, a window right above my medicine cabinet, and a dog that knocks things over. I’ve tried the amber bottle thing. I’ve tried the opaque sleeves. I’ve tried the foil. Half the time, I just forget. And honestly? I’ve been on the same glaucoma drops for five years. My pressure is stable. My vision is fine. So maybe the science is right, but the fear-mongering is overblown. Are there cases where degradation matters? Absolutely. But let’s not turn every medication into a sacred relic. I’ve seen people throw away perfectly good meds because they looked a little cloudy. That’s wasteful. That’s not caution-that’s anxiety dressed up as health literacy. I say: if it’s still in the bottle, still smells like medicine, and doesn’t have a fungus growing in it, use it. And if it doesn’t work? Then go see a real doctor. Not a blog post.