How to Confirm Pediatric Dosing on a Child’s Prescription Label
When your child gets a prescription, the label might say 10 mL. But that’s not the dose. The real dose is in milligrams. And if you miss that difference, you could be giving your child too much - or too little - medicine. This isn’t a guess. It’s a calculation. And getting it wrong can be dangerous.
Children aren’t small adults. Their bodies process medicine differently. A dose that’s safe for a 150-pound teen could kill a 20-pound toddler. That’s why every pediatric prescription must include two things: the child’s weight in kilograms and the exact dose in milligrams. Not milliliters. Not teaspoons. Milligrams. That’s the number that matters.
What You Need to See on the Label
Look at the prescription label. Does it say something like:
- Amoxicillin 400 mg (200 mg per 5 mL)
- Weight: 14 kg
- Dose: 20 mg/kg/day
If it only says “Take 10 mL twice daily” without mentioning milligrams or weight - stop. Call the pharmacy. This is a red flag. The FDA requires all liquid pediatric medications to show both metric (mg) and non-metric (mL) measurements. If it’s missing, it’s not compliant. And it’s risky.
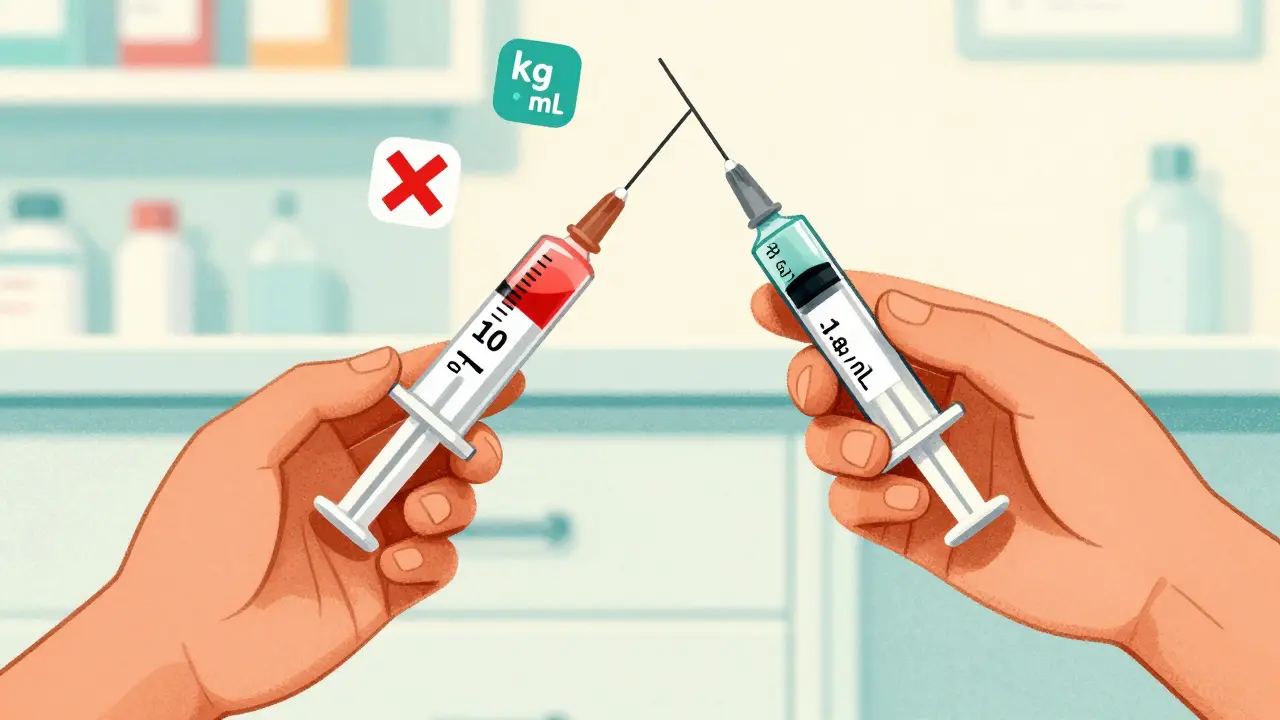
Parents often assume the number on the syringe is the dose. It’s not. The syringe measures volume. The label tells you how much medicine is in that volume. For example:
- Amoxicillin 80 mg/mL means 1 mL contains 80 mg
- Amoxicillin 40 mg/mL means 1 mL contains 40 mg
Same volume. Half the medicine. A 2x overdose if you use the wrong one. This mistake caused 37.2% of liquid medication errors in children under 2, according to the CDC’s 2021 Pediatric Medication Safety Report.
Do the Math - Even If You’re Not a Doctor
You don’t need to be a pharmacist to check this. Just follow three steps.
- Convert weight to kilograms - If the label says 30 pounds, divide by 2.2. 30 ÷ 2.2 = 13.6 kg. Round to 14 kg. This is the number used for dosing.
- Multiply weight by the dose per kg - If the dose is 20 mg/kg/day, then 14 kg × 20 mg = 280 mg total per day.
- Divide by frequency - If it’s given twice daily, 280 mg ÷ 2 = 140 mg per dose.
Now check the label: Does 140 mg match the amount in the volume you’re supposed to give? If the concentration is 80 mg/mL, then 140 mg = 1.75 mL. If the syringe only has markings for whole mLs, the pharmacist should have rounded it to 1.8 mL or 2 mL - and they must document why.
Don’t trust rounding unless you see it written out. Cerner and EPIC EHR systems automatically flag when doses are rounded. Pharmacists are required to note: “Ordered: 140 mg, Dispensed: 1.8 mL (rounded from 1.75 mL).” If that’s not on the label, ask.
Two Checks Are Better Than One
The American Society of Health-System Pharmacists (ASHP) says every pediatric dose needs dual verification. That means two people - usually a pharmacist and a nurse - calculate it independently. One person might forget to convert pounds to kilograms. Another might misread the concentration. Two calculations catch 94% of errors.
As a parent, you’re the third checker. Ask:
- “What is the exact dose in milligrams?”
- “Is this dose appropriate for my child’s current weight?”
- “Can you show me how to measure this with the syringe you gave me?”
These questions aren’t rude. They’re life-saving. A 2022 Reddit analysis of 1,247 parenting threads found 68% of parents felt unsure if the dose was right. One mother nearly gave her 4-year-old 10 mL of amoxicillin - thinking it was 10 mL of 80 mg/mL - when the correct dose was 200 mg total (2.5 mL). That’s a 2.5x overdose. She caught it because she asked.
Watch Out for These Common Mistakes
Here’s what goes wrong - and how to avoid it:
- Wrong weight conversion - Using 1 kg = 2 lb instead of 2.2 lb. This error caused 18.7% of miscalculations in a 2022 study. Always use 2.2.
- Confusing concentration - Amoxicillin comes in 40 mg/mL, 80 mg/mL, and 125 mg/mL. The bottle looks the same. The dose doesn’t. Always check the number after “mg/mL” on the label.
- Using Clark’s Rule - Some old charts say: “Weight in lbs ÷ 150 × adult dose.” That’s outdated. The American Academy of Pediatrics says direct mg/kg dosing is far more accurate. Don’t rely on old rules.
- Measuring with kitchen spoons - A teaspoon isn’t 5 mL. It’s often 4.5 mL. Use the syringe or cup that came with the medicine.
A nurse with 12 years in pediatric ICU told a forum: “The most dangerous situation is when parents see a dose that seems too small for an adult but don’t realize it’s correct for their child’s weight.” A 100 mg dose might look tiny - but for a 10 kg child, it’s perfect.

Technology Is Helping - But You Still Need to Check
Hospitals now use AI tools like DoseSpot’s Pediatric Safety Module, which checks doses against 15,000+ guidelines with 99.2% accuracy. EPIC and Cerner systems flag errors in real time. But these tools aren’t everywhere. Only 86% of children’s hospitals have full protocols. Just 43% of general hospitals do.
And even the best system can’t replace your eyes. A 2023 study found that 43.5% of preventable errors came from parents misunderstanding mg vs. mL. That’s not a tech problem. It’s a communication problem. You need to ask. You need to verify. You need to double-check.
What to Do If Something Doesn’t Add Up
If the label doesn’t have:
- The child’s weight in kg
- The dose in mg
- The concentration (mg/mL)
- A clear measurement device (syringe or cup)
Call the pharmacy. Ask for a corrected label. If they refuse, call the prescribing doctor. Don’t give the medicine until you’re sure. The Pennsylvania Patient Safety Authority found that 91.6% of pediatric dosing incidents were caused by calculation errors. Most were preventable.
The good news? The American Academy of Pediatrics now requires all pediatric prescriptions to include weight in kg and dose in mg - effective January 1, 2024. That’s a huge step forward. But until every pharmacy follows it, you’re still the last line of defense.
Remember: You know your child best. You know their size, their habits, their reactions. No algorithm or EHR system replaces that. Trust your instincts. Ask questions. Don’t be afraid to say, “I don’t understand - can you walk me through this?”
One mother caught a 3x overdose by comparing the label to the manufacturer’s dosing chart. She noticed the concentration on the bottle didn’t match the chart. She called the pharmacist. They apologized. They fixed it. Her child never got the wrong dose.
You can do that too.
What if the prescription only lists milliliters (mL), not milligrams (mg)?
If the label only says "Take 5 mL" without stating the dose in mg, the prescription is incomplete and unsafe. Ask the pharmacist for the exact milligram amount and the concentration (mg/mL). For example, "5 mL of amoxicillin 80 mg/mL" equals 400 mg. Without this, you can’t verify the dose is correct for your child’s weight. The FDA requires both metric (mg) and volume (mL) to be shown on pediatric labels. If they refuse to provide it, contact the prescribing doctor.
How do I convert my child’s weight from pounds to kilograms?
Divide the weight in pounds by 2.2. For example, a child weighing 33 pounds: 33 ÷ 2.2 = 15 kg. Always use 2.2 - not 2 or 2.5. Using the wrong number is one of the most common errors in pediatric dosing. Many pharmacies now enter weight in pounds and convert automatically, but you should still double-check the result. If the label says "Weight: 14 kg" but your child is 30 lbs, that’s incorrect - 30 lbs is 13.6 kg, not 14 kg. Ask them to confirm.
Why can’t I use a kitchen teaspoon to measure liquid medicine?
A kitchen teaspoon holds between 4.5 and 5.5 mL - not the standardized 5 mL used in medicine. That’s a 10% error, which can be dangerous for children. Always use the syringe, dropper, or dosing cup that came with the medication. These are calibrated to match the concentration on the label. If you lost it, ask the pharmacy for a new one - they’re usually free.
What’s the difference between mg/kg and mg/m²?
mg/kg (milligrams per kilogram of body weight) is used for most antibiotics, pain relievers, and common medications. mg/m² (milligrams per square meter of body surface area) is used for chemotherapy and some cancer drugs, where body size and metabolism matter more than weight alone. For most kids, you’ll only see mg/kg. If you see mg/m², ask the pharmacist to explain how it was calculated - it requires both height and weight. The Mosteller formula (√[height(cm) × weight(kg) ÷ 3600]) is the standard method.
Can I trust the dose if the pharmacy says it’s "standard"?
No. "Standard" doesn’t mean "safe for your child." Every child’s dose must be calculated based on their specific weight and condition. A "standard" dose for a 40-pound child might be lethal for a 20-pound child. Always verify the calculation using your child’s actual weight and the prescribed mg/kg. If the pharmacist says "this is what we always give," ask them to show you the math. If they can’t, get a second opinion.
Medication safety for children is a $287 million industry, driven by regulations and real-life tragedies. But the solution isn’t more technology - it’s more vigilance. You’re not just a parent. You’re a safety checkpoint. And your questions today could prevent a hospital visit tomorrow.



8 Comments
Dylan Patrick
March 14 2026One time I gave my kid 5 mL thinking it was 5 mL of 40 mg/mL when it was actually 80 mg/mL. Turned out to be a 2x overdose. I almost lost it. Never again. Always check the mg/mL. Always.
Kathy Leslie
March 15 2026I used to just eyeball it with a spoon until my pediatrician laid it out like this. Now I keep the syringe in my wallet. Seriously. It’s saved us twice. Don’t be like me - get the right tool.
Aaron Leib
March 17 2026The FDA requirement for dual labeling is non-negotiable. If your pharmacy gives you a label without mg and kg, they’re not just cutting corners - they’re risking a child’s life. Call the doctor. Demand a corrected label. This isn’t optional.
Elsa Rodriguez
March 17 2026I had a pharmacist tell me 'it's fine, we give this dose to every kid.' I wanted to scream. My 18-pound baby wasn't 'every kid.' I called the pediatrician at 2 a.m. They apologized. The pharmacy got shut down for three days. Don't let them gaslight you. You know your child better than they ever will.
Serena Petrie
March 18 2026Just use the syringe. Don't overthink it.
Amisha Patel
March 19 2026In India, we often get liquid meds without proper mg labeling. I had to learn this the hard way. Now I always write the dose on the bottle myself. It’s not ideal, but it’s safer than trusting the label.
Buddy Nataatmadja
March 19 2026I’m from Indonesia. We don’t have the same systems, but we do have community pharmacists who double-check with nurses. It’s not perfect, but it’s a start. Maybe we need more global awareness - not just better labels.
mir yasir
March 20 2026The assertion that 'parents are the last line of defense' is both empirically unsupported and socially regressive. Systemic solutions - automated EHR integration, standardized pharmacokinetic algorithms, and mandatory pharmacist certification - are the only sustainable approaches. Relying on laypersons to perform clinical calculations is a failure of institutional responsibility, not a commendable vigilance.